The life stories of two “Dayanands” reveal their indomitable courage. While the first Dayanand from rural Delhi died of cancer at the age of 39, the second Dayanand from East Delhi died of AIDS at the age of 46. What connects them was their use of alcohol, tobacco and other drug use; major risk factors of non-communicable diseases (NCDs).
Both the Dayanands had graduated from, what we call ‘The University of Pain’ and time and again had faced social rejection, stigma, and discrimination. They both volunteered to become peer support counselors and worked hard in empowering their peers. The Dayanand who died from cancer survived with two boys and his ageing mother. (To watch their stories click here)
Science knows about the correlation of cancer and alcohol use since the 1980s. The International Agency for Research in Cancer (IARC), the WHO’s research body, classifies alcohol as class one carcinogen since 1988.
“Indian society is losing more than it is gaining due to alcohol”
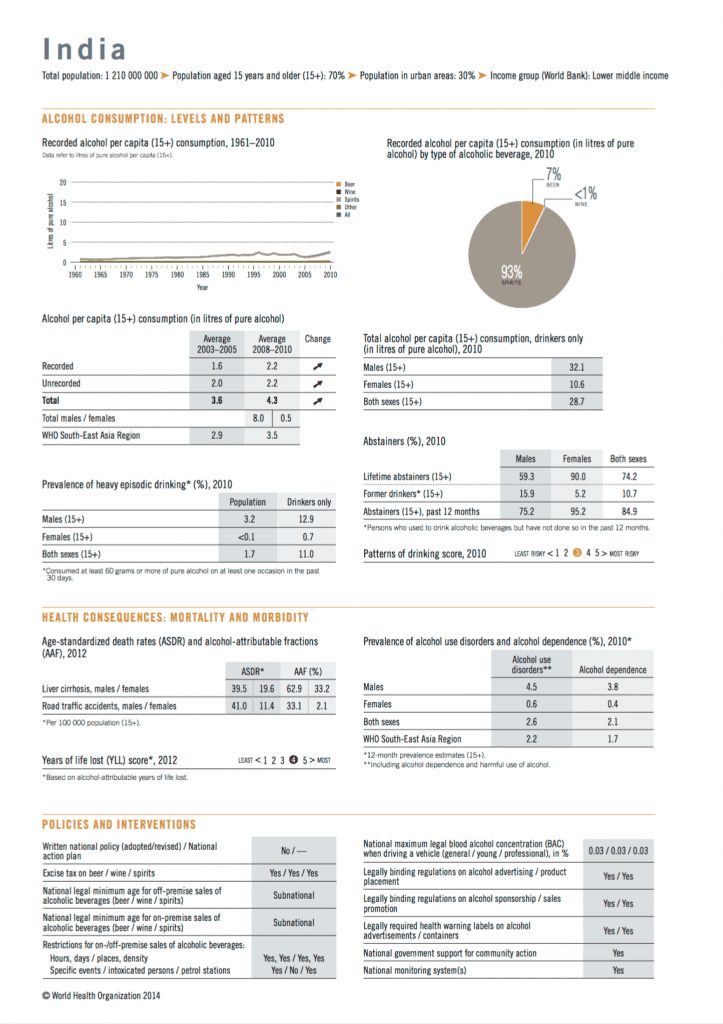
Alcohol can also significantly drain family budgets, since costs for NCD-related health care, medicines, and costs for alcohol diverts the household’s income and resources from ensuring food and nutrition security and from basic education. It is estimated that while gains in terms of revenue from alcohol sales in India are INR 216 billion every year, losses from the adverse effects of alcohol are estimated to be INR 244 billion, apart from immeasurable losses due to multiple and rollover effects of alcohol consumption (Gururaj, 2006) – this is a staggering fact, bearing in mind that 74% of Indian adult population choose to live free from alcohol.
One of the major burdens women are facing, is that of stigma and blame for alcohol and drug use of another family member, blame for hiding the issue from others and blame for not getting timely treatment.
Non-communicable disease in India
NCDs control programs have been vertical in India. There are separate programs for cancer, diabetes, cardiovascular diseases (CVDs), and others. The National tobacco control program in 42 districts and 21 states and the National cancer control program have been running for more than twenty years. Since 1984, Ministry of Health and Family welfare and Ministry of Social Justice have been working through NGOs to reduce the harm caused by alcohol, other drugs and tobacco. A person affected by disease remains the same but been dealt by different agencies under multiple programs at different times and different stages of the disease as health is a state subject.
- In India, NCDs are estimated to account for 60% of all deaths.
- India stands to lose $4.58 trillion before 2030 due to NCDs and mental health conditions. Cardiovascular diseases, accounting for $2.17 trillion and mental health conditions ($1.03 trillion), will contribute to major economic losses. This contrasts starkly with the cost of action: $111 billion a year to implement a set of NCD “best buy” interventions in all developing countries.
Healthy India Alliance
I was honored and glad to participate for NADA India and the IOGT International movement in the post WHO SEARO civil Society consultation round table meeting held at Public Health Foundation of India office. The meeting was convened by the NCD Alliance, organizing an Indian Civil Society Round table to deliberate on a collaborative CSO response to a Request for Proposals (RFP) for setting up a multi-disciplinary CSO coalition in India, to strengthen NCD advocacy. An ad hoc committee of organizations working on NCD issues in India responded to the RFP and volunteered to form the ‘Healthy India Alliance’ for the prevention and control of NCDs in India. Nada India Foundation joined the round table and later the Governing Board of the Alliance comprising 18 member organization covering four diseases and four risk factors.
To my mind, this was a timely meeting. It is, in fact, high time to come together as civil society and join efforts for preventing and reducing the NCD burden on India.
The Healthy India Alliance works with a mission to create an enabling environment for active participation of health and non-health Civil Society Organizations (CSOs) to prevent and control NCDs through effective policies, partnerships and programmes. Need has been identified to overcome the stigma and blame and should be associated with NCDs and its associated risk factors in order to empower and ensure the entitlement of the people effected and affected by NCDs to assert their right to health.
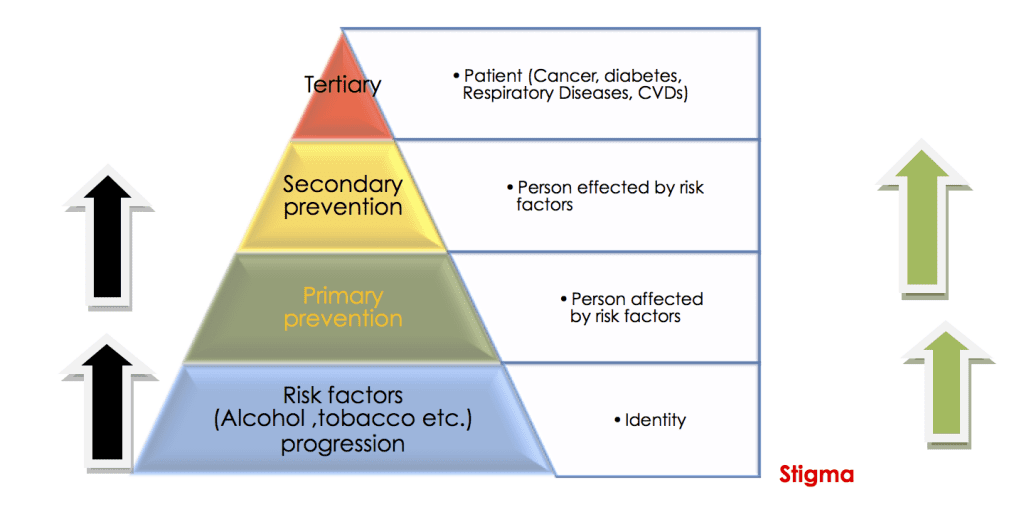
The adverse physical and mental health, social, environmental and economic consequences of NCDs affect all, particularly the poor and vulnerable populations. Nada India has been working on prevention of NCDs with a focus on alcohol and tobacco use at primary and secondary levels by using treatment readiness, peer based approach and capacity building of peer led rehabilitation centers.
Nada India as a member of the Healthy India Alliance sees it as an opportunity to build partnerships for strengthening systems related to alcohol prevention, treatment and rehabilitation in India. The best part of this alliance, as it builds upon the unique strengths of varied CSOs like Health Bridge, Indian Cancer Society, Pallium India, HRIDAY, Public Health Foundation of India, and many more, is to mobilize recourses and mitigate the health and socio-economic complexities arising from NCDs in India.
I see HIA as an engagement of multi-sectoral CSOs to tackle NCDs by generating awareness, building capacity, empowering people effected and affected by NCD and advocating for health promoting norms to reduce premature NCD mortality by 25% by 2025.
We are coming together to prevent NCDs in India.



