The Organization for Economic Cooperations and Development (OECD) has released the latest edition of the “Health at a Glance” report. Health at a Glance provides a comprehensive set of indicators on population health and health system performance across OECD member states and key emerging economies. These cover health status, risk factors for health, including alcohol, access to and quality of healthcare, and health system resources.
The report identifies smoking, alcohol use, physical inactivity and obesity as the root cause of many chronic conditions. For example, nearly one in five adults (19%) reported heavy episodic alcohol use at least once a month, on average, with rates over 30% in Germany, Luxembourg, the United Kingdom and Denmark.
The OECD analysis draws from the latest comparable official national statistics and other sources. Alongside indicator-by-indicator analysis, an overview chapter summarises the comparative performance of countries and major trends. This edition also has a special focus on digital health, which measures the digital readiness of OECD countries’ health systems, and outlines what countries need to do accelerate the digital health transformation.
Investing more in health systems contributes to gains in health outcomes by offering more accessible and higher-quality care. Differences in risk factors such as smoking, alcohol and obesity also explain cross-country variation in health outcomes. Social determinants of health matter too – notably income levels, better education and improved living environments.
Findings related to alcohol harm in the OECD
Alcohol use is a leading cause of death and disability worldwide, particularly among those of working age. High alcohol intake is a major risk factor for heart diseases and strokes, liver cirrhosis and certain cancers, but even low and small amounts of alcohol consumption increases the long-term risk of these diseases.
Alcohol also drives more car crashes and injuries, violence, homicides, suicides and mental health disorders than any other psychoactive substance, particularly among young people.
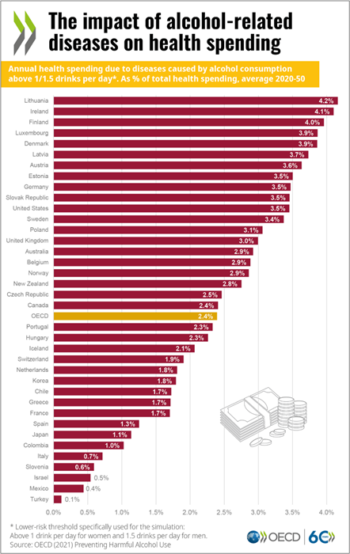
Alcohol-related diseases and injuries incur a high cost to society. An average of 2.4% of health expenditure is spent on dealing with the harm caused by alcohol consumption, and the figure reaches as high as 4% in some countries.
Alcohol-related diseases and injuries incur a high cost to society. Life expectancy is nearly one year lower than it would be, on average, if alcohol consumption in a population would be lower.
An average of 2.4% of health spending goes to dealing with the harm caused by alcohol consumption – and the figure is much higher in some countries. In addition, poor health due to alcohol consumption has detrimental consequences on labour participation and productivity.
Combined with the impact on labour force productivity, it is estimated that GDP will be 1.6% lower on average in OECD countries annually over the next 30 years, varying from 0.2% in Turkey to 3.8% in Lithuania.
Reduced productivity of employees amounts to US$ 595 billion (adjusted for purchasing power), according to the report.
Alcohol use prevalence across the OECD
Measured through sales data, overall alcohol consumption averaged 8.6 litres per person across OECD countries in 2021, down from 8.9 litres in 2011.
Latvia and Lithuania reported the highest consumption in 2021 (over 12 litres per person), followed by the Czech Republic, Estonia and Austria – all with over 11 litres per person.
Türkiye, Costa Rica, Israel and Colombia had comparatively low consumption levels (under 5 litres per person).
Among accession and partner countries, consumption was relatively high in Bulgaria and Romania (11 litres and over per person) and low in Indonesia, India and China (under 5 litres).
Average consumption fell in 23 OECD countries between 2011 and 2021, with the largest reductions in Lithuania and Ireland (by more than 2 litres).
Both countries have implemented high-impact and scientifically proven alcohol policy solutions in recent years.
However, alcohol consumption increased by more than 2 litres per person in Latvia, and by about 1 litre per person in Mexico and Norway, as well as in accession countries Bulgaria and Romania.
High-risk alcohol use across OECD countries
While national data on overall consumption per capita facilitate the assessment of long-term trends, they do not identify high-risk alcohol use patterns, such as heavy episodic alcohol use (also called binge alcohol use).
Nearly one in five adults (19%) reported heavy episodic alcohol use at least once a month, on average across 29 OECD countries in 2019. This proportion varies 10-fold, from less than 3% in Türkiye and Italy to more than 30% in Germany, Luxembourg, the United Kingdom and Denmark, as well as Romania.
The data presented herein may differ from estimates derived from other national sources. In all countries, men were more likely than women to report heavy episodic alcohol use.
On average across OECD countries, 26% of men reported heavy episodic alcohol use at least once a month compared to 12% of women.
Alcohol policy solutions
Policies to reduce alcohol use and prevent harm include broad-based strategies and those that target heavy alcohol use.
Comprehensive policy packages built on a “PPPP strategy” – pricing policies to limit affordability of cheap alcohol, policing to counter alcohol impaired-driving, primary care-based counselling for people with alcohol use disorder, and protecting children from alcohol promotion – are highly cost-effective in tackling harmful alcohol use.
Analysis of national efforts to prevent and reduce alcohol harm reveals that in many countries gaps remain in the development and implementation of proven policies.
These gaps persist in areas of alcohol policy making that yield the biggest return on investment and have the biggest cost-effectiveness, such as:
- Regulating the price of alcohol, through taxation and/ or minimum unit pricing,
- Limiting alcohol availability,
- Regulating alcohol marketing,
- Improving driving under the influence counter-measures,
- Improving screening and brief interventions, and
- Better regulating consumer information, for example through health warning labelling.
For example, alcohol has become cheaper in the OECD because of flawed alcohol taxation practices where governments fail to raise alcohol taxes adequately, to at least adjust alcohol taxation to inflation rates, and to ensure affordability decreases.
The OECD concludes that a comprehensive approach to alcohol harm, closing these gaps in alcohol policy development and implementation brings health benefits to the entire population, and helps save money. Whole of population
Two recent alcohol policy innovations are getting traction
Two recent innovative changes are emerging in the alcohol policy landscape.
One is the use of minimum unit pricing (MUP), which sets a floor price beneath which alcohol cannot be sold legally. MUP targets cheap alcohol that is consumed by heavy alcohol users and young people. MUP was introduced in Ireland in 2022, and is already in place in two of the United Kingdom nations (Scotland and Wales), and in some regions in Australia and Canada.
The second innovation is legislation mandating the labelling of alcohol products. While warning labels about the dangers of consuming alcohol while pregnant already exist in some countries, Ireland became the first country globally to mandate labels with population-wide health warnings on alcohol products (such as risk of cancers and liver diseases caused by alcohol).
Special OECD report on alcohol from 2021
Already in 2021, the OECD released a special report on alcohol harm and policy. It showed that investing in policies to prevent and reduce alcohol harm would save millions of lives. Implementing proven alcohol policy solutions would yield substantial returns on investment and would benefit the health care system, the economy and society overall.
Movendi International summarizes the main findings and comments on the report. And Movendi International recorded an Alcohol Issues Podcast episode with the main author of the report, Michele Cecchini.