In my last blog, I identified one of the unintended outcomes of using alcohol as an economic driver: it makes living an alcohol-free life more challenging, even when dining.
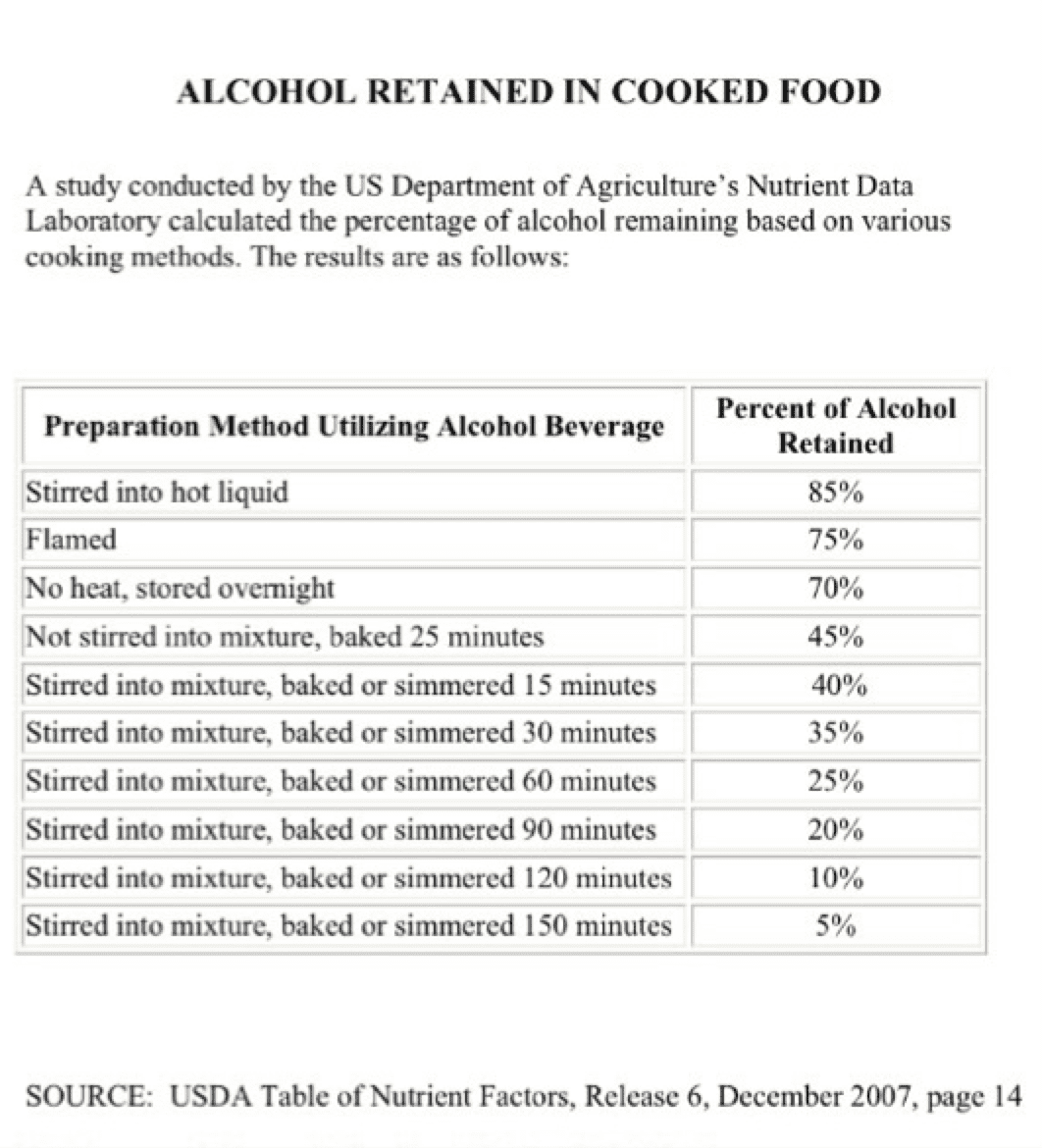
Craft beers, flavored beers, wines, and hard ciders are being used in foods ranging from bar-b-que to butter, and soups to soufflés. Most people are not aware that a significant amount of ethanol remains during most cooking methods. Just ask your server the next time you sit down to dine. Better yet, ask the chef. The myth that all the alcohol burns off is fairly pervasive. The following chart is from the U.S. Department of Agriculture. It shows how much alcohol is retained in various cooking methods.
From a policy and community standpoint, I’d like to offer a few thoughts for discussion and consideration. They are not concrete thoughts, by any measure. They are simply ideas that could be developed further in order to push back against the pervasiveness of alcohol in our culture.
Alcohol is a carcinogen. It is a Group 1 carcinogen (World Health Organization – IARC), meaning that it has been identified as a cause of cancer in humans. I did a little digging to find out how many items there are in the Group 1 carcinogen list that humans eat on purpose. There are five. Three are fairly regionalized in usage (Chinese style salted fish, plants containing aristolochic acid used in Chinese medicinals, and Areca (Betel) nut chewed South East Asian cultures). The fourth is processed meats, which is a new entry to the list. And then, we find alcohol. I wonder how many people know that there are only five Group 1 Carcinogens that humans eat on purpose? Furthermore, I wonder how many people know that an increasing number of recipes call for the use of a known carcinogen (alcohol) in their food?
When I’m the prude at the table requesting that my meal be prepared without alcohol, I know that I’m avoiding a carcinogen. I am familiar with the recent research showing the shocking number of alcohol attributable cancer deaths in my country (20,000 per year). I doubt that folks at the tables around me are aware that the wine in their meat sauce, the beer in the batter of their onion rings, the champagne in their butter, and the rum in their dessert provides them with multiple exposures to an added group 1 carcinogen.
So, here is my musing on potential policy directions.
How would it look if advocates from public health, cancer organizations, food safety, healthcare, addiction services, mental health services and others came together to demand accountability for group 1 carcinogens added to foods? If a regulation exists that says we must know the calorie, fat, sugar and sodium content of labeled foods, shouldn’t we also know the group 1 carcinogen content? If restaurants are required to warn patrons of potential food allergies and dangerously hot coffee to avoid law suits, how much more sense would it make to warn patrons about which foods contain a group 1 carcinogen?
What would it look like if recovery groups (and other who wish to live an alcohol free life) began a media campaign edifying restaurants with the highest percentage of group 1 carcinogen-free food. Do you think that would make a ripple in the food universe? They wouldn’t be calling establishments out for using too much alcohol, they’d simply be cheering the restaurants that choose to leave that particular ingredient aside.
Of course, slowing down the juggernaut of the alcohol industry and its strangle hold on governments who only see a tax dollar to be gained by additional sales would not be an easy task.
However, the word “cancer” means something to the public at large. It has a different feel than the typical words we use when addressing the expansion of alcohol availability; binge alcohol use, driving under the influence, overdose, cirrhosis, etc. It’s easy to pass those off if they are fairly out of the circle of your experience. We all eat food. And if we eat food with alcohol, we’re being exposed to unnecessary risk. Even if policies or laws can’t be created to address it, we can at least find ways to provide education to dining public. It’s worth it to help lower risk and improve public health.
